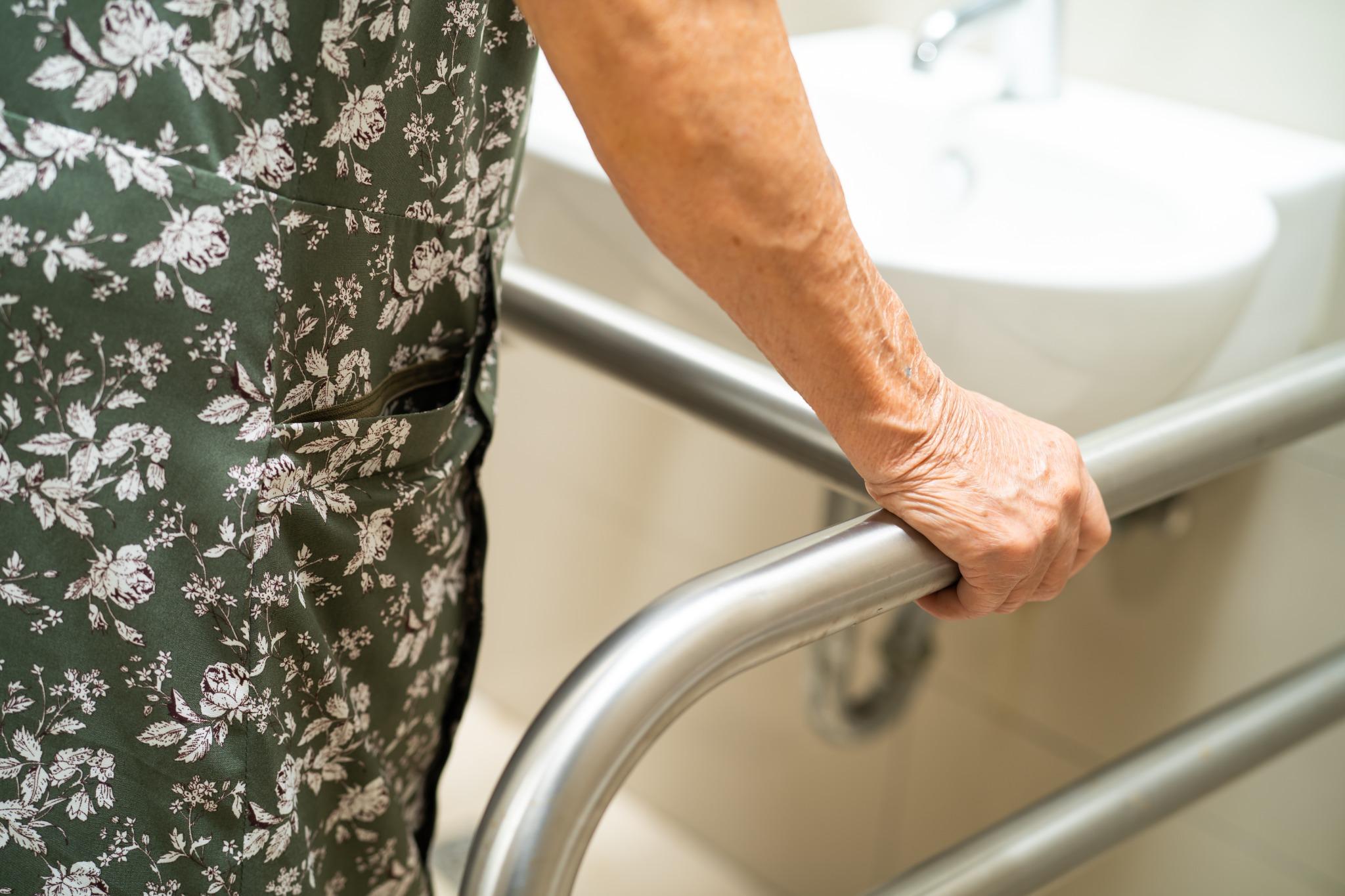
Introduction
Long-Term Patient Independence is the goal most patients share when they return home after surgery, illness, or a life-changing diagnosis. The ability to move safely, manage daily routines, and stay connected to familiar surroundings can dramatically improve quality of life. Yet independence rarely comes from a single product. It comes from thoughtful coordination between rehabilitation equipment, home accessibility solutions, and reliable ongoing support.
Medical equipment providers play a critical role in shaping that experience. When equipment, home modifications, and maintenance services work together, patients gain the confidence and stability they need to remain safe and active at home.
Here are six practical ways providers can strengthen Long-Term Patient Independence:
• Build complete support ecosystems instead of selling standalone products
• Combine rehabilitation equipment with home accessibility improvements
• Align equipment with each patient’s clinical and functional needs
• Expand services with user-focused solutions and partnerships
• Maintain continuous follow-up instead of one-time installations
• Prioritize reliable repair and maintenance systems
The following insights from healthcare professionals and industry leaders show how providers can shift from equipment vendors to long-term partners in patient independence.
Build Ecosystems, Not Products, to Strengthen Independence
Many providers focus heavily on the equipment itself. A wheelchair, lift chair, or rehabilitation device is selected, delivered, and installed. While these tools are valuable, they only tell part of the story.
True Long-Term Patient Independence begins when providers view equipment as part of a larger living system. Patients recovering or managing chronic conditions often face daily obstacles that extend far beyond the device they were prescribed.
Niclas Schlopsna, Managing Partner at spectup, explains:
“From what I have observed working with healthcare related startups and service providers, long term patient independence improves when medical equipment providers stop thinking in terms of single product sales and start thinking in terms of a support ecosystem. Many patients managing care at home need more than a mobility aid or rehabilitation device. They need coordinated solutions that help them move safely, access daily spaces, and maintain confidence over time.”
Schlopsna describes a provider that initially focused almost entirely on rehabilitation devices. The products were high quality, yet many patients struggled months later because their homes were not set up for the equipment.
“Once the company began offering home accessibility assessments alongside the equipment, small changes like ramps, grab bars, or better bathroom access dramatically improved how well patients could use their rehabilitation tools. The equipment suddenly became part of a complete living solution rather than an isolated purchase.”

Niclas Schlopsna, Managing Partner
In other words, independence doesn’t come from the device alone. It comes from the environment supporting that device.
Providers who build coordinated systems help patients move through their homes safely, reduce fall risks, and maintain the routines that make daily life manageable. When equipment, home modifications, and service support work together, patients experience stability instead of frustration.
Unite Equipment, Home Mods, and Reliable Support
Healthcare professionals often see the consequences when these elements are not aligned. A patient may receive a high-quality assistive device but struggle to use it effectively because their home environment was never evaluated.
Dr. Martina Ambardjieva, MD, urologist and medical expert at Invigor Medical, emphasizes that independence requires integrated planning:
“Long-term patient independence is best supported when medical equipment providers move from a product-delivery model to a longitudinal care-support model. For patients managing care at home, especially older adults and those with neurological, postoperative, mobility, or continence-related limitations, independence depends on the integration of specialized rehabilitation equipment, home accessibility solutions, and responsive technical support.”
She notes that providers create the most value when equipment recommendations reflect the patient’s medical condition, mobility level, and home environment.
“From a clinical standpoint, providers add the most value when they align equipment recommendations with the patient’s functional status, medical condition, caregiver capacity, and home environment. This includes not only mobility and transfer aids, but also solutions that reduce fall risk, support hygiene, preserve dignity, and improve adherence to home-based care routines.”
Equally important is dependable service.
“Delayed repairs, poor fit, or equipment failure can rapidly contribute to complications, including falls, skin injury, infection risk, caregiver burden, and avoidable hospitalization.”

Martina Ambardjieva, Medical expert
A well-designed home care system accounts for all of these variables. When providers assess the home environment, educate patients and caregivers, and maintain responsive support, Long-Term Patient Independence becomes much more achievable.
Expand Care Solutions with User-Focused Design
Another opportunity lies in expanding product and service offerings to better reflect the realities of home-based care.
Many patients need multiple solutions working together. Mobility aids, therapy equipment, bathroom safety tools, and adaptive home modifications often intersect during recovery or chronic care management.
Michael Kazula, Director of Marketing at Olavivo, highlights how a broader care approach benefits both patients and providers:
“Medical equipment providers can boost long-term patient independence by integrating specialized rehabilitation products, home accessibility solutions, and ongoing support services. This comprehensive approach not only aids patients in their recovery but also opens up valuable opportunities for affiliate marketing within the healthcare sector.”
At its core, the strategy centers on patient experience. Instead of offering isolated products, providers can curate equipment systems that meet real daily needs.
Kazula explains that this approach starts with diversification and thoughtful design.
“Key strategies include diversifying product ranges and focusing on user-centric designs to meet varied recovery needs.”

Michael Kazula, Director of Marketing
In practice, this might include pairing rehabilitation equipment with adaptive home features, offering guidance on installation, or connecting patients with complementary support services.
Patients benefit from having fewer gaps in care. They spend less time searching for separate solutions and more time focusing on recovery and daily life.
For providers, the result is stronger relationships with patients and caregivers. That continuity often leads to better outcomes and long-term loyalty.
End Transactional Care with Continuous Follow-Up
One of the most common gaps in home care support appears after equipment has already been delivered.
Patients leave the hospital with devices designed to help them function independently. Yet weeks or months later, many providers have little or no contact with them.
Dr. Mariam Zakhary, Clinical Advisor at Ikon Recovery Center, sees this pattern regularly.
“The biggest issue is that providers treat equipment as a transaction. A patient gets a wheelchair, grab bars are installed and that’s it. Rehabilitation equipment, home modifications, and service support have to be planned together for long-term independence at home, starting from day one, with the real home environment assessed before anything is ordered.”
Follow-up plays a major role in Long-Term Patient Independence because patient needs evolve.
“Most providers fail to follow up. Conditions change, equipment breaks down, and a patient who got everything right at discharge can lose independence within months if nobody checks in.”
Regular check-ins can reveal small issues before they escalate. A device might require adjustment. A patient might stop using a tool because it feels uncomfortable or inconvenient.
“As an LCPC and NCC, I see this clinically too. Patients stop using their adaptive equipment and nobody notices until there is a crisis.”

Dr. Mariam Zakhary D.O., Clinical Advisor
LinkedIn, Ikon Recovery Center
Providers who stay connected to clinical teams and patients catch those signals earlier. That continued involvement helps patients maintain the routines and confidence needed to remain safely at home.
Sell Systems and Deliver Reliable Uptime
Equipment reliability is another critical piece of Long-Term Patient Independence.
A single malfunctioning device can disrupt an entire care routine. If a lift chair stops working or a mobility aid requires repair, the patient’s independence can quickly deteriorate.
Dr. Gregg Feinerman, Owner and Medical Director at Feinerman Vision, frames the issue in terms of system performance.
“Instead of just selling products, sell a system of independence. A wheelchair isn’t just a wheelchair, a transfer bench isn’t just a transfer bench, when its picked for someone’s home along with their stair rail, bedside commode and therapy equipment.”
The reliability of that system becomes the real product.
“When a provider sells or installs 3 or 4 pieces of equipment but doesn’t think about repair issues, the whole system grinds to a halt because of one malfunctioning piece.”
Providers that build maintenance and service response into their care model create stability for patients.
“Conversely, however, long-term system reliability skyrockets when the provider checks all the boxes: product selection, installation, caregiver training and repair response within 24-48 hours.”
Feinerman describes this concept simply.
“I like to think that uptime is our product.”

Dr. Gregg Feinerman FACS, Owner and Medical Director
When equipment works consistently, patients can move through their day without interruption. That consistency builds trust and strengthens independence over time.
Own Outcomes with Rapid Service and Home Retrofits
The strongest providers take responsibility not only for equipment delivery but also for the long-term results of the solutions they install.
Dr. James Lyons, Clinical Advisor at Epiphany Wellness, argues that independence requires an adaptive mindset.
“The vast majority of equipment providers treat patients like one time transactions. That’s the problem.”
He explains how quickly patient needs can change.
“Someone comes home after a stroke and is handed a wheelchair and a grab bar, and then nothing. No follow-up. No adjustment six months later when their condition changes again.”
True Long-Term Patient Independence requires responsiveness.
“To a moving target you do not prescribe a static solution. A person needs mobility at month three and a person needs mobility at month eighteen.”
Providers who succeed treat patient care like a continuous process rather than a fixed installation.
“Better outcomes for me have been from providers that think of pit crew, not car dealerships. Quick. Responsive. Always changing.”
Lyons also highlights the importance of home accessibility retrofits.
“But ramps and grab bars and widened doorways are not luxury add-ons either. This is what keeps someone out of a nursing home.”

Dr. James Lyons, M.D., Clinical Advisor
When equipment, home modifications, and service support work together, patients gain a dependable system designed to evolve with their needs.
Conclusion
Long-Term Patient Independence does not come from a single device or one-time installation. It develops through thoughtful coordination between rehabilitation products, accessible home environments, and dependable service support.
Providers who move beyond a transactional model and focus on systems, follow-up care, and reliable repairs create stronger outcomes for patients and caregivers alike. When equipment works within the patient’s real living environment and remains supported over time, independence becomes sustainable rather than temporary.
The future of home healthcare will belong to providers who see their role not simply as equipment suppliers, but as long-term partners helping patients maintain dignity, mobility, and Long-Term Patient Independence in the place they most want to be: home.