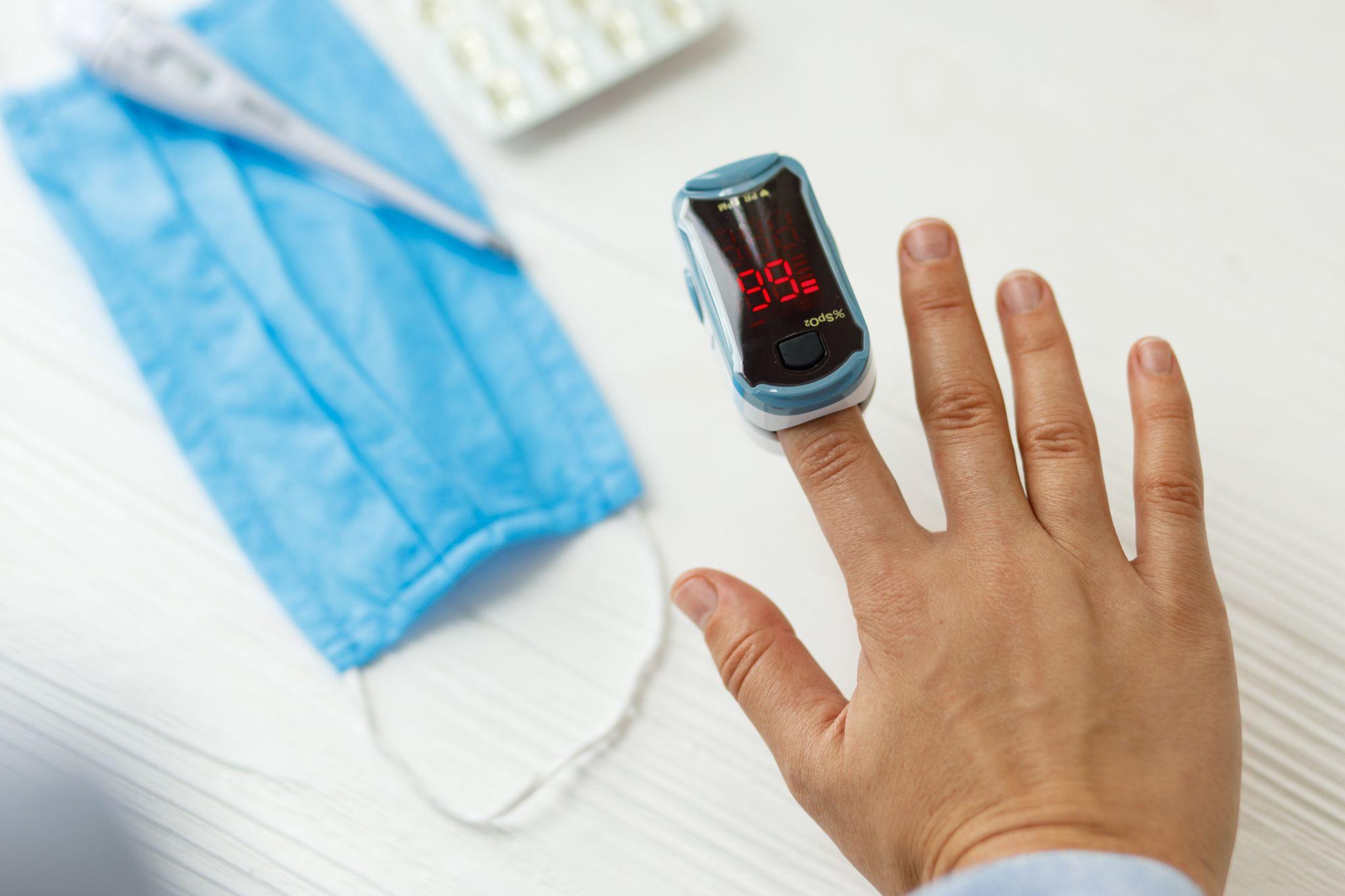
Person using crutches indoors, representing essential medical product delivery supporting patient mobility and recovery.
Delivering essential medical products isn’t just about moving boxes. It’s about trust. Providers rely on timely deliveries to treat patients safely, stay compliant, and control costs. One missed shipment or expired lot can ripple across an entire care team.
In this roundtable on essential medical product delivery , four leaders shared the operational and supply-chain decisions that made the biggest difference in reliability and responsiveness.
Here’s a quick look at the key takeaways:
- Prequalify backup suppliers to avoid single points of failure
- Tie safety stock levels to real demand signals like appointment pipelines
- Automate FEFO and lot control to reduce waste and audit stress
- Take ownership of logistics to prevent delays and customer disputes
Each approach balances inventory availability, compliance requirements, and cost control in a different way. Let’s take a closer look at how these decisions play out in the real world.
Prequalify Backup Suppliers to Strengthen Essential Medical Product Delivery
One of the clearest reliability wins came from building supplier redundancy. Instead of depending on a single vendor, organizations maintain pre-approved secondary and tertiary suppliers. That shift alone reduces vulnerability during disruptions.
When a primary supplier hits a delay, procurement teams can pivot immediately. There’s no scramble to vet paperwork, no last-minute compliance review. Orders simply move. That speed protects essential medical product delivery in moments when providers can’t afford uncertainty.
Cost control still plays a role. Not every SKU needs three suppliers. High-risk or high-impact items get layered protection and higher stock buffers. Lower-risk products remain cost-optimized. This segmentation keeps capital from being tied up unnecessarily.
Compliance stays intact because every supplier is pre-qualified in advance. Switching vendors doesn’t create regulatory exposure. Instead of reacting to crises, the supply chain becomes structured around resilience. It’s a shift from fragile dependency to built-in flexibility.

Mr Shashi Shekhar, CEO
LinkedIn, Gobookmart media pvt ltd
Use Demand Signals to Set Smarter Safety Stock Levels
In medical aesthetics, supply interruptions damage more than schedules. They damage trust. One franchise leader shared how moving away from just-in-time ordering for core injectables and consumables changed everything.
The breakthrough came from tying safety stock directly to the three-week appointment pipeline. Instead of guessing, they forecast based on booked procedures. Their top five SKUs now carry rolling safety stock aligned with confirmed demand.
Yes, it required more upfront capital. Expiration tracking became more important. But reschedules due to supply shortages dropped to nearly zero. In essential medical product delivery, that kind of reliability strengthens patient loyalty and referrals.
Compliance remained non-negotiable. Lot numbers, storage temperatures, and expiration dates are tracked in shared systems. Audit readiness isn’t an afterthought. At the same time, predictable volume allowed for better distributor negotiations. Waste fell through disciplined stock rotation and proactive flagging of near-expiration inventory.
The result is a balanced system. Availability supports patient experience. Compliance protects licensure. Cost is controlled through smarter forecasting rather than aggressive lean practices that create risk.

Ryan Pittillo, Owner
LinkedIn, ProMD Health Bel Air
Automate FEFO and Lot Tracking to Reduce Waste and Audit Risk
Manual lot tracking across thousands of SKUs invites errors. One medical distribution client solved this by automating FEFO, or first-expired, first-out, picking through custom system scripts.
Expired inventory write-offs dropped from roughly 7 percent to under 1 percent in six months. That kind of improvement transforms the financial picture. In fact, the client increased safety stock on critical items by 15 percent because reduced waste freed up cash.
Automation also strengthened compliance. Lot numbers, temperature logs, and chain-of-custody documents attach directly to shipments. Audit preparation shifted from week-long scrambles to pulling structured reports in minutes.
Order fulfillment speed improved as well. Warehouse staff no longer manually checked expiration dates on every pick. That time savings improved responsiveness without sacrificing accuracy.
For essential medical product delivery, automation becomes more than an efficiency play. It protects patient safety, reduces regulatory exposure, and creates room in the budget for strategic inventory buffers.

Louis Balla, VP of Sales & Partner
Control Logistics to Improve Responsiveness and Reduce Disputes
Another leader made a bold call: take full control of logistics. Instead of making clients coordinate rental equipment returns, they include prepaid overnight return labels and absorb shipping costs upfront.
On paper, that sounds expensive. In practice, it eliminated most late-return disputes and equipment sitting idle in customer offices. Responsiveness improved because inventory cycles became predictable.
The company also prioritized depth over breadth. Rather than stocking one of everything, they invested in multiple units of their most in-demand equipment. That decision required roughly $75,000 in standing inventory, yet utilization climbed sharply. When three clients need the same unit at once, the answer is yes.
Compliance and cost control were reinforced by becoming preferred distributors for key brands and servicing equipment in-house. Faster repairs reduced downtime and built long-term trust.
This approach highlights an important truth about essential medical product delivery. Sometimes spending more in targeted areas lowers overall friction, reduces hidden costs, and increases reliability.

Lisa Reeves, President
LinkedIn, Environmental Equipment and Supply
The Real Takeaway on Essential Medical Product Delivery
Across all four examples, one pattern stands out. Reliability doesn’t come from cutting inventory to the bone. It comes from intentional decisions about where to build buffers, where to automate, and where to take ownership.
Balancing inventory availability, compliance requirements, and cost control isn’t about choosing one over the others. It’s about structuring essential medical product delivery so each supports the next. When systems are designed for visibility, redundancy, and accountability, responsiveness follows naturally.
That’s what turns a supply chain from reactive to dependable.